IBS: Irritable Bowel Syndrome
IBS is a common condition, but it can be hard to pin down as it is considered functional. This is in contrast to structural conditions, in which a sign would be there to find through imaging, biopsies, or other tests. However, this is not to say that IBS is not real.
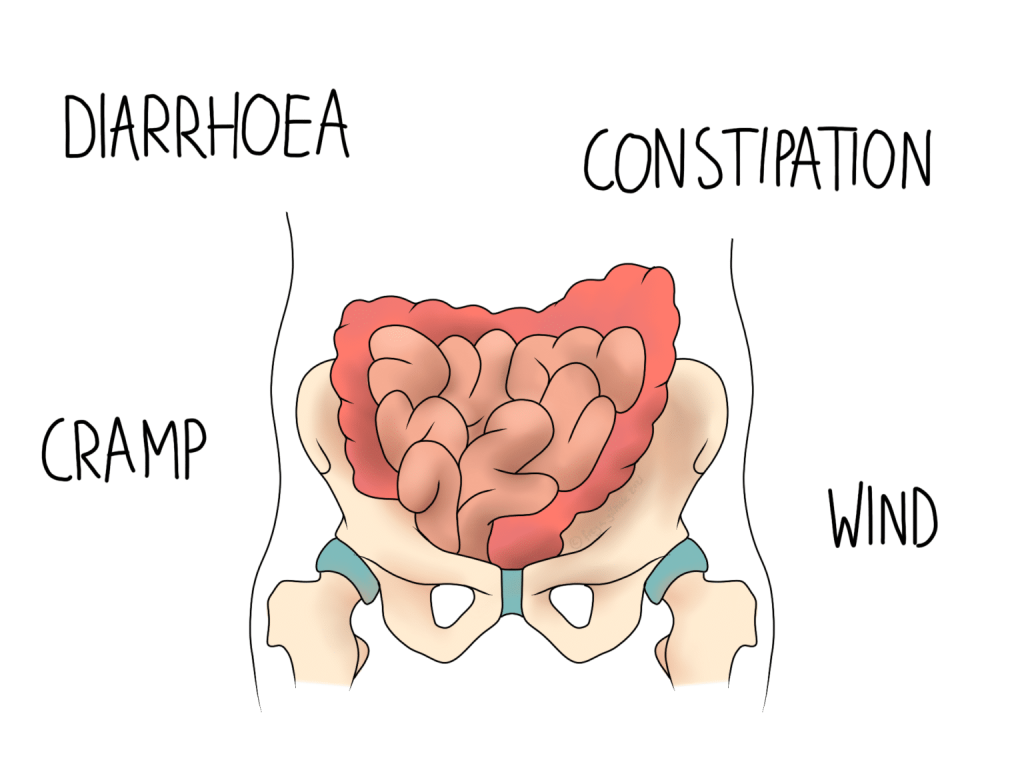
IBS Basics
The condition is characterised by:
- Abdominal cramps
- Bloating
- Diarrhoea
- Constipation
Sometimes it can be difficult to spot a pattern, or you may find that stress or certain foods trigger them. It can become a vicious cycle when the stress and anxiety of potential symptoms actually aggravates them further.
Some people find that they develop back pain alongside IBS flare ups, which can be a direct referral from the digestive system rather than a back problem as such. Therefore, osteopaths need to be aware of the symptoms of IBS and how we may be able to help a patient manage them.
Diagnosis
As the condition is functional, any diagnostic tests are performed to rule out other conditions. There are similarities with conditions that require treatment and monitoring such as ulcerative colitis and Crohn’s disease. Not to be confused, they are under the umbrella of IBD. This stands for Inflammatory Bowel Disease, and can be life threatening if not managed properly.
Your GP may also use blood tests to check for deficiencies. These are more likely when the body is not absorbing nutrients properly, such as IBD or IBS where diarrhoea is significant. Be sure to mention if your diet does not contain a specific food group, such as vegetarianism or veganism. B12 deficiency is more common in people who do not consume animal products, so special effort may need to be made to ensure adequate intake of certain nutrients.
Osteopathy and IBS
The ASA recognises that osteopathy can help with some issues of digestion. A research study has also shown that there may be benefit to patients with IBS to have manipulative treatment to the spinal joints (“clicking”). Clicking joints has a local effect on the joint, muscles, and nerves, so a possible explanation for this is that the click calms down the nerves that supply the bowel. This may just provide temporary relief, but sometimes taking the edge off helps to wind down the cycle of anxiety and IBS. Thinking mechanically like this, your osteopath may also want to treat further up the back in case there is a relationship between a lower back that is overworking and the nerves mentioned above.
Stress is often an aggravating factor for IBS. We can help with the effects of tension, which you may find helps to break the stress cycle somewhat. There is also a relationship between the diaphragm, which typically tightens up with chronic stress, and the digestive system. We know that the diaphragm has a direct effect on reflux as its normal function supports the sphincter at the top of the stomach. For people whose IBS symptoms involve stomach symptoms (such as increased burping), this could be a useful avenue to explore in clinic.
Make an appointment in Leicestershire or Rutland here for digestive issues.