Shin Splints
Avin has a special interest in sports injuries, of which shin splints are a common example.
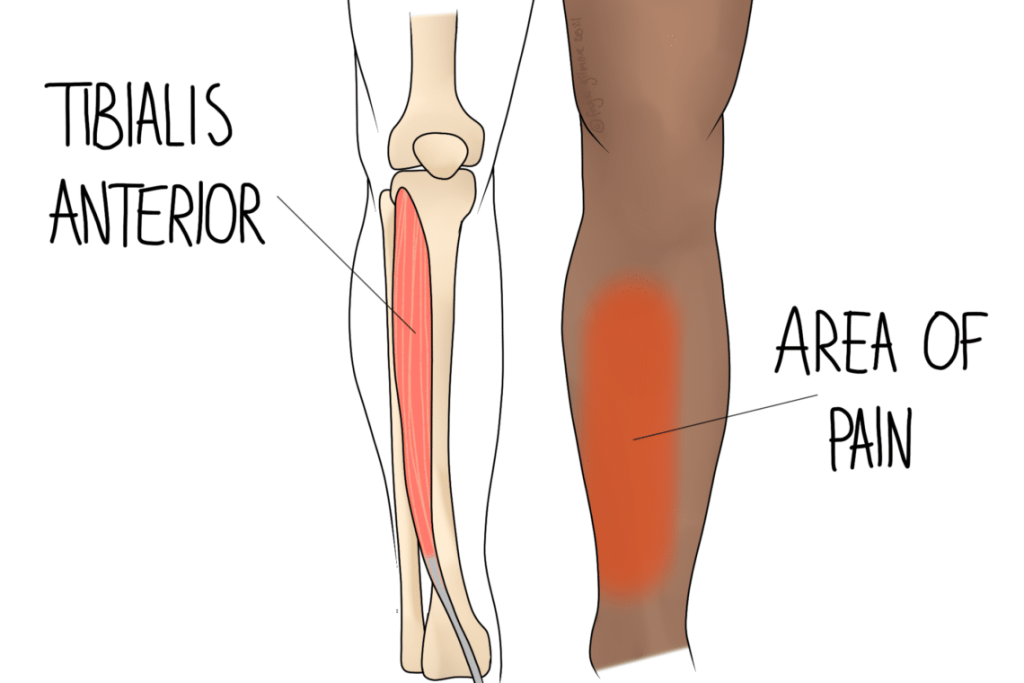
Symptoms of Shin Splints
Also known as Medial Tibial Stress Syndrome, symptoms affect the inner side of the shin. Pain may come on at the start and end of exercise, disappearing in between. As it gets worse, pain may persist through the day. There will be an area on the shin that is tender to press into, and there may also be some slight swelling over the same area.
Running is commonly associated with the development of shin splints, but other sports can cause them too. The exact science of what happens anatomically is unclear, but there is a link with repetitive high force from the muscle onto the bone. Powerful movements such as jumping are also associated.
It is important to note that this is not the same as a stress fracture. However, a stress fracture may follow if the condition and its cause are not managed. Although the two have similar symptoms, initially a stress fracture will feel better after rest, whereas shin splints will feel worse.
The muscles around the shin bone (tibia) are involved in shin splints. Their role is to move the ankle, which explains why running and jumping are the common causes. Typically, there is an inflammatory reaction where these muscles meet the bone. This may involve inflammation of the outer layer of bone itself, or it might be the connection between the muscle and bone.
Prevention of Shin Splints and First Aid
We know that shin splints tend to come on when either:
- an action is performed incorrectly
- too much is done in too short a period
So when thinking about prevention, we need to be thinking about form and graded exposure.
There is also a connection with running on hard surfaces, or with poor shock absorption from inadequate footwear. Proper running shoes that are replaced after about 300 miles may help. If possible, running on softer ground might also help to prevent the development of shin splints.
As the condition is involves inflammation, a cool compress is ideal for first aid. You never aim to numb the area, just to cool it down. This takes the edge off the swelling and pain without hindering the healing process. The NHS has advice for painkiller use here.
Your Osteopath’s Role
The appropriate management will depend on how soon you come to clinic after your injury. A brief period of rest is recommended in the first few weeks. After this period, we can support you in graded return to your chosen exercise. This might mean running for shorter distances, or running fewer days per week. We may also ask you to choose a flatter, more even surface in this phase.
As always, we will also look elsewhere for other relevant factors. For example, if your ankle movement was restricted, the muscles may have to work harder to perform the action you’re trying to do.
Your osteopath may be able to help you with your training programme, or put you in touch with someone who can. If the problem has been that you have overloaded the area, we can help with strengthening and rehabilitation.
You can book an appointment here to start managing shin pain.